The most commonly occurring cancer in the US among women is breast cancer. Statistics point to how 1 in 8 women in the US develops breast cancer. Many different types of breast cancer are there which vary in terms of the spreading or metastasis to different body tissues. The causes of breast cancer are equally varied. Breast cancer is diagnosed at the time of a physical exam. Self-examination of the breasts, ultrasound testing, mammography and biopsies are some of the ways to detect this disease. Treatment of breast cancer depends on type of cancer and the stage and involves chemotherapy, radiation or surgery.
As per the American Cancer Society, close to 250,000 fresh cases of invasive breast cancer are diagnosed among women in 2017 and over 2,400 in men. Close to 40 thousand women and 440 men succumbed to breast cancer in the year 2015. With close to over 3.1 million American breast cancer survivors in the US, breast cancer and survival has risen in the US for different races and a worse survival rate for certain communities. The America Cancer Society indicates that yearly mammograms for those aged 45 to 54 for women at risk for breast cancer and mammograms every couple of years and yearly screening for those 55 years or older.
Breast cancer is characterized by the growth of a malignant tumor arising from breast cells. Though this form of cancer affects women, it can also occur in men. Breast cancer is not so common in men with around 2400 cases diagnosed annually in the US. But for those men afflicted by this disease, late diagnosis often causes metastasis and impacts prognosis. Breast cancer is noted in men aged 60 or more. For women, the common symptoms range from a lump in the breast to change in breast tissue skin or nipple discharges.
Kinds of Breast Cancer
Table of Contents
There are various kinds of breast cancer, with some more commonly occurring than others. There are also a blend of cancerous symptoms.
- Ductal Carcinoma (In Situ): This is considered one of the most noninvasive breast cancers and does not spread so easily. As a result, the prognosis for this category of cancer is remarkably good.
- Invasive Type Ductal Carcinoma: This disease begins at the breast ducts and enters the adjacent tissue. It is a commonly prevailing form of breast cancer with 80 percent breast cancers of the invasive type being that of ductal carcinoma.
- Invasive Type Lobular Carcinoma: This is the outcome of cancer in the breast glands that secrete milk. Close to 10 percent of invasive type breast cancers are of this category.
Less common types of breast cancer are covered below.
- Mucinous Carcinoma: This is formed from mucus secreting cancer cells. Various tumors comprise numerous types of cells.
- Medullary Type Carcinoma: This is a breast cancer that infiltrates structured boundaries between non cancerous and cancerous tissues.
- Triple-Negative Breast Cancer: There are various kinds of invasive cancers with cells lacking progesterone and estrogen receptors and no increase in the protein named HER2 on the surface. It occurs in younger women.
- Inflammatory Breast Cancer: This cancer creates redness and gives off heat from the breast skin, making it appear as a form of infection. The blockage of lymph vessels by cancer cells are changes noted here.
- Paget’s Disease: This impacts the breast ducts and reaches the nipples and the area adjacent to it. It is associated with crusting, and nipple redness.
- Adenoid-Cystic Type Carcinoma: These cancers have cystic and glandular features. The cancer in question is not very aggressive and is associated with positive prognosis.
- Lobular Carcinoma (In Situ): This leads to invasive breast cancer.
Other more unusual types of cancer are phyllodes tumor, papillary carcinoma, tubular carcinoma and angiosarcoma.
Various Pictures of Breast Cancer
Fig 1:- Different Areas Of Breast
Fig 2:- Progression Of Inflammatory Breast cancer
Image Source: cancersurvivalrates.net
Fig 3:- Various Stages Of Breast Cancer
Image Source: breastcancerstages.org
Causes of Breast Cancer
There are many different risk factors that lead to breast cancer. While many of these are known, how they impact the development of the cancer cell and the cause of the cancer is something less light has been shed on. On account of mutations in the DNA, normal breast cells become cancerous and while many are genetic, others result from DNA changes to breast cells acquired during one’s life.
Proto-oncogenic factors help in cell growth. If there is cell mutation, the growth of the cells can rise without any limit. These mutations are called oncogenes and such uncontrolled cell growth leads to cancer. Certain breast cancer risk factors can be modified such as alcoholic intake, whereas others like advancing age cannot. It is critical to discuss the risks with healthcare providers when new therapy begins. Many risk factors are not conclusive while others such as alcohol usage are clearly defined.
Here are the predisposing factors that trigger breast cancer.
#1 Demographical Characteristics
Photo by: Fiona Kilfoyl/ CC BYAdvancing age signals increased chances of getting breast cancer. The risk of breast cancer is more among women with relatives having this disease. A close relative with cancer increases the risk of women more than 2 times. Personal history is another indicator and potential risk factor. It increases the risk of cancer in the other breast or the chance of cancer in the original breast as well.
#2 Predisposing Factors
Women having benign breast conditions have increased chances of developing breast cancer. This is inclusive of atypical hyperplasia, where breast cells proliferate, but no cancer grows. Women starting their menstrual cycle at an age younger than 12 or going through menopause after 55 also show more chances of developing this disease.
Additionally, women with dense breast tissues as shown by the mammogram have higher chances of developing breast cancer. White women have a higher risk of breast cancer development, and African American women have more aggressive tumors when breast cancer develops. Additionally, exposure to chest radiation or use of diethylstilbestrol raises the risk of breast cancer. Additionally, late pregnancy or no children raise the risk of breast cancer as well. Another risk of breast cancer results from breastfeeding for one and a half to 2 years. Use of oral contraceptives in past 10 years raises the risk of breast cancer as well. Combined hormone therapy post menopause also raises chances of contracting this disease.
Other factors include alcohol intake, with recent studies showing even light drinking can aggravate breast cancer. Additionally, exercise lowers the chance of this cancer. Genetic risk factors include mutations in BRCA1 and BRCA2 genes. These are the breast cancer and ovarian cancer genes. Inheritance of a mutated gene from parents means a higher chance of developing breast cancer.
#3 Genetic Factors
Doctors are aware that breast cancer occurs when cells grow in an abnormal way. Cells dividing more rapidly as opposed to healthy cells continue to accumulate, forming the mass or lump. Cells spread through metastasis through the breast to lymph nodes as well as in other body parts. Breast cancer results when the milk creating ducts are impacted. Breast cancer may also begin in the lobules or glandular tissue or other cells or tissue within the breast.
Identification of hormonal, environmental and lifestyle factors that up the chances of cancer of the breast are easy. Yet the question as to why some people are more prone to this disease than others lies in the genetic factors. Breast cancer is caused due to an interaction in a complex way between nature and nurture. It is estimated by doctors that close to 5-10 percent of breast cancers are linked to genetic mutations passing through familial generations.
Numerous inherited mutated genes increasing the possibility of contracting breast cancer have been located. The most well known of these are breast cancer gene 1 or BRCA1 and breast cancer gene 2 or BRCA2. These raise the chances of developing breast and ovarian cancer respectively. If one has a strong genetic or medical history of breast or other forms of cancer, a blood test can be recommended to locate specific mutations in the BRCA or other genes passed along the family.
You also need to check with the doctor for a referral to genetic counselors, who review familial medical history. Genetic analysts also isolate the risks, benefits, and limitations of genetic testing to assist with shared decision making.
Among the factors that trigger breast cancer are the women with breast or ovarian cancer previously or those with even non malignant lumps. Many with no risk factors also develop breast cancer. Family history is as important as advancing age. A woman with a sister, daughter or mother who is affected is as much as 3 times likelier to develop breast cancer. This likelihood rises if more than a single first-degree kin has been affected. The genes responsible for familial breast cancer need to be understood. The genes BRCA1 and BRCA2 are directly implicated. Around 1 in 200 women carry these genes. Having a single one predisposes women to breast cancer, but does not directly cause it.
#4 Hormonal Factors
Women aged 50 or above are more susceptible to breast cancer as opposed to younger women. Additionally, African American females are more likely to develop breast cancer during the premenopausal period. The link between hormones and breast cancer is well established. The greater the exposure to the hormone estrogen, the more prone one is to breast cancer. Hormone estrogen enables cells to divide and the more they do so, the more they are possibly abnormal and cancerous. A woman’s exposure to progesterone and estrogen increases and decreases during the lifetime. It is influenced by the age one starts and stops menstruating, the age at the first birth and the duration of the menstrual cycle. The risk for breast cancer rises if one starts menstruating prior to age 12, has the first child post age 30, stops menstruation after age 55 or has a shorter or longer menstrual cycle than 26 to 29 days.
Greater chance of developing breast cancer stems from early ingestion of birth control pills. The risk dissipates if one has not used birth control pills for at least a decade. Certain studies suggest that opting for hormone replacement for menopause with a combination of estrogen and progesterone may raise the risk factor, especially when taken for more than 5 years. Heavy radiation therapy doses may also be a factor, though mammograms that are low dose pose no risk whatsoever.
#5 Diet Factors
The association between breast cancer and diet has been debated. Critical risk factors are obesity and drinking alcohol on a regular basis, and these can trigger the disease. Research has shown that women with high-fat diets are more certain to develop the disease. If a woman lowers daily calorific intake from fat that is 30 percent or lower, the diet can offer protection from breast cancer development.
#6 Age Factor
Likelihood of developing breast cancer rises as one’s age advances. This condition is more likely among women over 50 who have undergone menopause. Around 8 in 10 cases of breast cancer occur in ladies above 50 years of age. Women who are 50-70 years of age need to be screened for breast cancer regularly. Women above the age 70 can also be screened through GP or local screening units.
#7 Family History
Those with breast or ovarian cancer affected relatives may have a higher risk of development of breast cancer. As breast cancer is most common in women, it occurs in more than a single family member if there is previous medical history. Many cases of breast cancer may not run in families but genetic factors influencing breast cancer development can be passed on to children from parents.
Freshly detected genes such as TP53 and CHEK 2 are also linked with rise in breast cancer. If there are 2 or more relatives from one side of the family who have developed breast cancer under 50 years of age, surveillance for breast cancer or genetic screening for genes that make breast cancer development likely come into play.
#8 Benign Lumps or Dense Breast Tissues
If a person has had breast cancer before, or early cancerous changes in cells of breast ducts, the chances of getting the disease again are high. Benign lumps can also signal an increased chance of developing breast cancer. Certain benign changes such as cells in ducts growing abnormally or pathological cells inside breast lobes can lead to an onset of this disease. The breasts are made of lobules that generate milk. This glandular tissue contains a larger concentration of breast cancer cells than other tissues, adding to the density. Women with dense breast tissues have greater chances of developing breast cancer as more cells become cancerous.
Dense breast tissues can make a breast mammogram tough to read, as any lumps or abnormal tissues are tough to detect. Younger women have dense breasts. As age advances, the glandular tissues decrease and fat deposits, so breasts decrease in denseness.
#9 Exposure to Estrogen
Female hormone estrogen can stimulate breast cancer cells, triggering growth. The ovaries where eggs are stored produce estrogen when puberty commences, so periods are regulated. As the amount of estrogen, the body is exposed to rises, the risk of developing breast cancer may rise slightly. For instance, if a woman starts her periods early and ends with late menopause, estrogen exposure over a period of time is longer. Not opting for children or having children later can raise breast cancer risk because estrogen exposure is not impacted by pregnancy,
#10 Hormone Replacement Therapy
Hormone replacement therapy is linked to higher chances of developing breast cancer. Combined HRT and estrogen-only HRT raises the chance of developing breast cancer, though the risk is higher if combined HRT is opted for. With additional 19 breast cancer cases for every thousand women taking combined HRT for a decade, the risk rises if hormone replacement therapy is taken, but returns to normal when it is no longer taken.
#11 Birth Control Pills
Ingestion of oral contraceptives also raises the chance of developing breast cancer. Risks associated with birth control pills fall once the pill is no longer taken and the risk of breast cancer returns to normal after a decade of stopping.
#12 Obesity
If one has experienced menopause and prone to obesity, there is a risk of developing breast cancer. This is likely linked to the estrogen in the body. Being overweight or heavy can cause more estrogen secretion post the menopause.
#13 Alcohol
The chance of developing breast cancer can rise with the alcohol amount taken. Research shows there are more tendencies to develop breast cancer, with close to 200 women having 2 alcoholic drinks per day increases the risk of developing this disease by three more women as against those who do not take drinks.
#14 Radiation
Medical procedures using radiation such as CT and X-rays increase the risk of developing breast cancer too. If one has radiotherapy to the chest area for diseases like Hodgkin Lymphoma, there are greater chances of developing breast cancer later.
#15 Gender
Being a female is a major risk factor for breast carcinoma. Women are 100 times more prone to breast cancer, as opposed to men.
#16 Obesity
Another causative factor when it comes to breast cancer is obesity. Overweight and obese women are at increased risk of developing breast cancer, post-menopause. The risk level rises with rising body weight.
Symptoms of Breast Cancer
If you have a sharp, acute breast pain accompanied with tenderness, a breast lump or nipple discharge, these are signs and symptoms of breast cancer. Though breast cancer manifests no symptoms early on, timely detection can serve as a life-saving measure. Pain or tenderness in the breast is not the first obvious symptom of breast cancer, however.
Early Signs & Symptoms
Signs of breast cancer also include a change in the nipple shape, breast pain that does not abate after the next period, a new lump that does not go away post the period or clear, red, yellow or brown nipple discharge from a breast. Additionally, lack of redness, swelling, itchiness, rash on the breast or skin irritation is another sign you need to be alert. Breast cancer is also signaled by a lump or swelling around the collarbone or under the arm.
Additionally, lumps with irregular edges are most possibly cancerous.
Later Signs & Symptoms
Later breast cancer signs include the inward turning of the nipple or retraction, breast enlargement, dimpling of the surface of the breast, a lump that increases in size and an orangeish peel texture to the skin. Additionally, lots of weight loss, vagina pain or enlarged lymph nodes in the armpit and visible breast veins are later signs of this form of cancer.
Symptoms: A Summary
Photo by: Cancer Research UK/ CC BYHaving one of the above signs or symptoms does not mean one has breast cancer. For example, nipple discharge can also be the result of an infection. The leading symptom of breast cancer for most women and men is a lump or thickened tissue in the breast. Most breast lumps are not cancerous, but medical attention is critical to rule this out.
Seek medical attention if you notice any one of the following:
- A change in the size/shape of one or both breasts
- A new lump or thick tissue in one, or both breasts not there before
- Bloody nipple discharge
- Lump or swelling in the armpit
- Dimpling of breast skin
- Rash on or around the nipple
- Change in the appearance of the breast and its parts
- Swelling in collarbone or armpit
A change in shape, feel or size of the breast is one of the key symptoms of breast cancer. Breasts may look bigger or have a shape that is unusual when breast cancer sets in. Apart from breast pain, skin changes can also signal breast cancer. These include dimpling, puckering, rash or redness of the breast. The skin may appear to be an orangeish peel or have a texture that feels different. Nipple discharge and leakage can also be a symptom if you aren’t pregnant or breastfeeding. A rare breast cancer is inflammatory breast cancer where the breast reddens and inflames and feels sore. Underlying breast cancer can also manifest through Paget’s disease in the form of a red, scaly type rash.
Invasive breast cancer can cause irritated or itchy breasts, change in the shade and coloring, increase in breast shape or size, changes in touch, breast lump or thickening and redness or pitting of the breast skin. How breasts feel and look is an important part of health. Screening tests can find breast cancer in early stages before the appearance of symptoms.
A new lump or mass that is painless and hard with irregular edges is more likely to be cancer. Swollen lymph nodes need to be checked by medical professionals to ascertain if a lump or swelling is there. As mammograms do not detect cancer every time, it is essential for you to know signs and symptoms of cancer. Many women do not have obvious symptoms when breast cancer is detected.
Once symptoms are diagnosed, symptoms are an important part of cancer treatment and care. This is also known as symptom management.
Detection
It is important to have regular breast exams by doctors for which purpose mammograms are recommended. Breasts need to be checked for any suspicious changes. To know and examine your breasts for any changes is therefore important when it comes to averting or detecting breast cancer in time. Apart from regular self-breast exams, you need to be alert about the shape or breast symmetry. Self-exams can be carried out and imaging tests may also be required.
According to the American Cancer Society, women between 40 and 44 years of age should have annual mammograms screening if they prefer. Women aged between 45 and 54 should have a mammogram every year and those 55 years or above should opt for mammograms 1-2 years. According to the Task Force for US Preventative Screening, women and men should test for breast cancer every 2 years from age 50 to 74 and conduct annual screenings for mammograms. A mammogram shows breast lumps close to 2 years before they can be detected. Different tests determine if lumps can be cancerous. Imaging tests like ultrasounds and mammograms often detect the difference.
Doctors can also do a surgical biopsy and needle aspiration to collect and test tissues for cancer cells. When diagnosed with breast cancer, it becomes essential to know the type and degree of advancement. The lymph nodes can be checked to ascertain if the disease has spread. Tests can provide an indication of which treatment works best.
Tests and procedures used range from breast exam to ultrasound, mammogram or X-ray of the breast and samples of breast cells for testing or biopsy. Breast MRI will also detect this condition. Tests and procedures to assess the stage of breast cancer include blood tests, mammograms, bone scan, breast MRI, CT and PET scans.
Not all patients require all the tests. Some of these can be adequate to detect the stage and degree of advancement easily. Breast cancer stages range from 0 to 4, with the former indicating that it is non-invasive or contained within milk ducts. Stage 4 breast cancer also known as metastatic breast cancer is when the cancer is aggressive and has spread to other body parts. Breast cancer staging also takes the cancer grade into account, apart from tumor markers, and receptors for HER2, progesterone, and estrogen as well as proliferation factors.
If you want to prevent problems, you need to increase detection skills and breast cancer tests fall into one of the following categories.
Screening tests such as annual mammogram are routinely provided to those who are healthy and not suspected of breast cancer. The aim is to detect cancer early before symptoms manifest and cancer is easier to manage.
Diagnostic tests like biopsy are provided to those suspected of having breast cancer, on account of symptoms experienced or screening tests. This determines if breast cancer is present or not and whether it has traveled to other parts of the body. Diagnostic tests can be used to get more information about cancer to make treatment decisions.
Monitoring tests are another category. Once breast cancer is diagnosed, tests are used during and post the treatment to assess how the therapies are working. Monitoring tests can also check for recurrence.
#1 Biopsy
Imaging studies such as MRI and mammogram along with physical breast exams can help doctors to assess if a person has breast cancer. Tissue samples need to be taken from the affected area and examined under the microscope as part of biopsy. The biopsy is a small operation to remove the tissue from the affected area. If the doctor detects a problem, he or she may order a biopsy. The tissue sample is examined by pathologists to check if cancer cells are there or not. If the cancer is detected, the pathologist can report the characteristics.
A biopsy is a simple process. In the US, close to 20 percent of women who have biopsies are able to detect cancer in time. In Sweden, the percentage is closer to 80. Different biopsy techniques can be used so that the least invasive procedure possible will be used. Smallest incision and least scarring can be the result. The procedure depends on individual differences. A biopsy can be carried out by placing the needle through the skin to remove the tissue sample. Minor surgical procedures can also be carried out, in which the skin is cut through by the surgeon to remove suspicious tissues.
Fine needle aspiration biopsy is the least invasive of these methods, with zero scarring. An ultrasound-guided biopsy can be used or a stereotactic needle biopsy in case mammograms are used. Core needle biopsy uses a massive hollow needle as opposed to fine needle aspiration. In case the lesion cannot be felt through the skin, the radiologist or surgeon can use this image-guided technique to detect cancer. Mammotome or MIBB is a vacuum-assisted breast biopsy is a fresh way to perform a biopsy of this bodily area. Also, a form of breast biopsy is incisional biopsy which is like normal surgery. Excisional biopsy is surgery that removes the entire area of the tissue affected from the breast. It is one of the best ways to establish a definitive diagnosis without obtaining false negative results.
#2 Blood Cell Count
Both prior and post the treatment for breast cancer, doctors can order blood cell counts. Tests can be checked to ascertain if the blood has usual levels of blood cell types. Cancer can prevent the normal blood cell level your body needs to function effectively. Blood cell counts measure the following:
Leukocytes or white blood cells which function as the immune system’s defenders against foreign bodies and invaders. If there is low WBC count, there is likely to be an infection.
Erythrocytes or red blood cells carry oxygen across different parts of the body. Additionally, the number of red blood cells can be measured to assess the level of hemoglobin, a protein that is iron rich and found in blood cells which carries oxygen to different parts of the body from the lungs. When there are low hemoglobin levels, anemia can also result. Tests are needed to measure hematocrit level, of the entire blood volume comprising the red blood cells.
Thrombocytes or platelets are cells which prevent bleeding through clot formation.
Post the commencement of treatment, blood cell counts may be used to assess if another medical state like anemia can be addressed. A deviation in counts indicates that the bone marrow now has become infected with cancer. Prior to each treatment cycle, the blood cell counts need to be checked with different chemotherapy levels.
If counts remain low, medications called growth factors must be stimulated by certain blood cell types. Another option is transfusion that involves transference of healthy blood/blood components into the body.
Post the treatment, blood testing can be used to assess signs of recurrence and monitor medication side effects. White blood cells or immune cells and platelets are taken till they return to normal. Doctors order blood counts on an occasional basis, depending on the nature of the treatment.
#3 Blood Chemistry Test
The blood chemistry tests measure certain blood substances to indicate if organs are healthy and functional or not. Tests can measure liver enzymes and bilirubin, the former being proteins involved in chemical reactions and the latter being a substance cutting down on fat, for liver function evaluation. Additionally, levels of chloride, potassium, and urea nitrogen levels reflect liver health and kidneys pre and post the treatment. Additionally, calcium levels determine kidney and bone health. Blood glucose levels are important for those with diabetes and individuals taking steroids apart from medication to counter inflammation. Deviations in blood chemistry indicate that breast cancer spreads to the bone or liver. Doctors may also order imaging studies.
#4 Markers
Doctors may also order blood tests for tumor markers or cancer, for detecting cancer-oriented activities in the body. Proteins and tumor cells circulating are the markers that have to be measured. A cancer tumor provides a specific blood protein that serves as a cancer marker. Circulation of tumor cells are cells that edge away from the cancerous growth and go to the bloodstream. Markers that can be measured include proteins and circulating tumor cells.
Blood marker tests can be carried out prior to treatment for diagnosing the breast cancer and assessing if it has moved to other body parts at the time of treatment. Assessing whether the cancer is responsive and post-treatment, and recurrence are other evaluation measures. Markers used to assess breast cancer and detect it include CA 15.3, TRU QUANT, CA 27.29, CA125 and CEA as well as circulating tumor cells. Markers can also serve as early indicators of breast cancer stage and recurrence. If one has an elevated marker, markers periodically assess responses to treatments like chemotherapy.
#5 Bone Scans
A bone scan is known as scintigraphy. This is an imaging test to assess if breast cancer travels to the bones. The bone scan may also be ordered to check the bone health and create baseline images at the initial point of diagnosis. Pre and post the treatment, persistent joint and bone pain or breast cancer metastasis can be assessed. Bone scans commence with radioactive material injection into the arm, taken by bone making cells over the next few hours.
Bone scans commence with radioactive material in the arm, taken by the body’s bone making cells post the next few hours. These bone making cells are found in disease-damaged areas, and the new bone is being used to patch holes. Areas of additional bone activity show that radioactive substances collect new bone formation areas. Areas appear as dark film patches, so different parts of the bone can be impacted by cancer.
The bone scan is painless and involves less radiation exposure, creating no risks other than standardized X-ray. Changes in the spine need more evaluation and assessment. Bone scans cannot be used for noninvasive breast cancer. Bone scans only work if the persistent pain is detected.
#6 MRI
Magnetic Resonance Imaging or MRI is a technology using radio waves and magnets to create a cross-sectional imaging on the body’s inner side. MRI does not involve the use of X-rays, as it does not create radiation exposure. Breast MRI has numerous functions for breast cancer, including testing high-risk women, gathering information about the area of suspicion on the ultrasound or mammogram, monitoring treatment post-recurrence.
#7 Physical Exam
Manual exam of breasts or a breast physical examination can be tested by doctors and health professionals. This exam indicates the lumps that can be found with their own self-examinations. The abnormalities in the breast can be tough to feel. So breast physical exams are needed under medical supervision. Lumps, asymmetry or thickening or changes in the breast may be detected by medical professionals more effectively. If one is treated for breast cancer, breast physical exams need to be carried out 3-4 months. Frequently scheduled physical exams decrease in frequency as treatment escalates.
#8 Breast Self Exam
The breast self-exam can be used for examining breasts on their own. It is a vital way to find breast cancer earlier, and treatment post the detection. Every cancer cannot be found this way. BSE is a useful screening strategy when combined with physical exams on a regular basis and mammography. Close to 20 percent of the time, breast cancer can be discovered by physical exams. Breast exams are routinely performed as part of screening strategies.
#9 CT Scans
A CT or CAT scan or computerized tomography scan is an X-ray method that provides information about the internal organs in two-dimensional slices or cross-sectional divides. At the time of CT scan, one lies on a moving table and passes through a machine that takes X-rays from different perspectives and angles. CT scans cannot be routinely used to evaluate the breast, however. If there is large cancerous growth, the CT scan can be ordered to assess if cancer has moved into the chest wall. This determines whether cancer can be cured with mastectomy. Doctors can order CT scans to examine different parts of the body where breast cancer has metastasized such as lungs, lymph nodes, liver, spine or brain. CT scans would not be required if one has an early stage breast cancer. If the symptoms or other findings indicate cancer could be advancing, more CT scans may be ordered. Researchers are also investigating if the breast CT scans could be a more optimal screening tool as opposed to traditional mammography. At the time of breast CT, one lies face down on the table while the scanner rotates around the breast. The dose of radiation is akin to a conventional mammogram.
#10 Chest X-Rays
Before commencing treatment for invasive or advanced breast cancer, the chest X rays will be used to check if cancer has spread to the lung area. The test is used for assessing heart and lungs prior to the receipt of chemotherapy or general anesthesia. During treatment for breast cancer, chest X rays can be used for different situations such as advanced breast cancer spreading to the lungs, the presence of pneumonia, or inflammation of the lungs.
#11 Digital Tomosynthesis
This is a method approved by the US FDA but not considered a standard of care for breast cancer screening as it is new. Digital tomosynthesis of the breast differs from that of the standard mammogram in the way similar to a CT scan of the chest differing from a standard chest X-ray. It’s like the differences between a ball and a circle. Mammography takes two X-rays of each breast from various angles namely top to base and sideways. In a mammogram, breast tissue appears as irregular areas with white shading called shadows
Digital tomosynthesis involves overcoming big issues such as taking multiple X-rays for each breast across different angles. The breast is positioned the same way as a conventional mammogram, though less pressure is applied. The X-ray tube moves in an arc around the breast while images are taken at a 7-second examination. Information is transmitted to the computer where it is assembled to yield clear, highly focused 3-D images through the breast. Earlier results with digital tomosynthesis are positive.
#12 Ductal Lavage
Ductal lavage is a fresh technique used for detecting pre-cancer and cancerous breast cell changes in those at risk for developing this disease. Ductal lavage involves doctors applying suction to the nipple to bring out fluid from tiny ducts. This fluid is evaluated through a technique called pap smear. This test offers an early warning about the signs of cancer. The exact location is needed to complete the biopsy. Ductal lavage is followed by other tests like imaging studies.
#13 EndoPredict Test
This test is one of the genomic tests for those diagnosed with estrogen receptor positive, early-stage HER2 negative breast cancer. This EndoPredict test can be used to make treatment decisions based on the risk of cancer coming back to the part of the body further from the breast or distant metastasis within 10 years post-diagnosis. This genomic test also provides a risk score which can help women and their doctors. Genomic tests study the cancer tumor to ascertain how active specific genes are. The genetic activity level affects the behavior of cancer, including how likely it is to undergo metastasis. Genomic tests help in making decisions about whether treatment post surgery will be beneficial.
#14 FISH Test
This stands for Fluorescence in-situ hybridization which maps the gene-based material in the cell of the person. This test is suited for the visualization of certain genes or their portions. FISH tests are carried out on breast cancer linked tissue collected at the time of biopsy to check if cells have more copies of HER2 genes. The more copies there are, the wider the number of receptors the cells possess. HER2 receptors give off signals indicating the spread of breast cancer.
This test will tell you if cancer falls under positive or negative, reported as zero for HER2.
FISH testing one of the many methods of HER2 testing called IHC. FISH is regarded as accurate. Labs do IHC tests first, ordering the other test only if IHC results do not show whether cells are HER2- or +. Certain HER2 testing results may not be right. This is because different labs show the disparity in the classification of positive and negative HER2 status. The FISH test is best performed on tissue preserved in chemicals or wax.
#15 IHC
IHC (also known as ImmunoHistoChemistry) is a specific staining process carried out on breast cancer tissue removed either fresh or frozen at the time of biopsy. IHC is tested to demonstrate whether or not cancerous cells come with HER2 receptors or hormone receptors on their outer base. This plays a vital role in planning and managing treatment. This method of detecting cancer checks if the tumor has excessive HER2 receptor proteins on the cancer cell surface, instructing the cells to grow and replicate.
The IHC test provides a score ranging from zero to three plus that measures HER2 hormone receptor protein on the cell surface in the breast cancer tissue. If the score ranged from 0 and 1 positive, it is known as HER2 negative and scores of 3+ or more are HER2 positive. In between, 2+ is borderline. Research has indicated that HER2 testing results can be erroneous, for example, if HER2+ is the case, but results show it as negative, or vice versa, this can cause a problem in treatment or diagnosis.
#16 Genomic Tests
Different types of genomic tests analyze the activity of specific genes in early stages of breast cancer. The tests can be applied to make treatment decisions and ascertain the chance of cancer recurring within ten years post the diagnosis. If a woman has a high or low risk of early stage breast cancer, chemotherapy or other treatments can lower risks once the surgery is required.
#17 Mammograms
These are important tools doctors have to screen for breast cancer and diagnose as well as evaluate and follow those who have had breast cancer. Safety and reasonable accuracy apart, the mammogram is an X-ray photograph of the diseased area. This technique has been used for over 50 years. For those patients at average risk, mammograms should be screened at the start at age 40 to assess the breasts for early signs of breast cancer. If there is a higher risk of breast cancer, mammograms may be performed at a younger age. Diagnostic mammograms differ from screening mammograms when it comes to gaining information about certain areas of concern, such as a mammogram or suspicious lumps. Diagnostic mammograms take more images as opposed to those used for screening.
#18 Mammostrat Testing
This is another genomic test, that measures five certain genes in cells of breast cancer. This can be used to assess in case cancer also has a high or low chance of recurrence. Being aware of whether a woman has high or low risks of early-stage breast cancer coming back can help women and their doctors o assess if chemotherapy or other treatment can reduce risk post surgery.
#19 MarginProbe
This method uses electromagnetic waves to isolate potential cancerous tissues. This method was developed to assist surgeons in judging how much tissue should be removed at the time of a lumpectomy. It is less likely women need surgery post lumpectomy if this method is used. At the time of lump removal, cancerous tumor and margin surrounding it are operated. If the margin contains cancer cells, the test is said to be positive. Surgeons learn the status of the margin before the completion of the lumpectomy, so tissues can be removed after cleaning the margins. Analysis of the removed tissue takes over a week. Post the pathology report, margins contain cancer cells and additional surgery or re-operation is needed. In under 3-5 minutes, the MarginProbe system detects subtle differences between normal tissue and affected cells using electromagnetic radiation. The MarginProbe test also clarifies if more tissue should be removed.
#20 Molecular Breast Imaging
MBI (also called Molecular breast imaging) is a breast cancer detection method. This is also called the Miraluma test, sestamibi, breast specific gamma imaging, and scintimammography. This test uses a radioactive tracer lighting up cancer ridden areas within the breast. This tracer injects through the body via veins in arms. Breast cancer linked cells contain more radioactivity than normal cells. MBI has a lot of promise when it comes to detecting breast cancer, especially in those with above average chance of disease and dense breasts. A study conducted by Mayo Clinic in the year 2008 found that dense breasts were easier to monitor and cancer could be faster detected through MBI than mammography.
#21 PET Scans
PET scans, also known as Positron Emission Tomography, detect cancer areas by getting images of body cells as they function. This procedure is simple, as the breasts are injected with radioactive sugar which tends to be absorbed in a greater rate by cancer-ridden cells. Additionally, the special camera scanning the body picks up highlighted spots on the screen of the computer. This helps in identifying where cells are active, indicating cancer. Doctors should know where to look and further evaluation can then be carried out with different techniques. This is inclusive of the PET and CT scan in some centers.
PET scans can also be used to evaluate people post breast cancer to check if the disease has spread to lymph nodes, other parts of the body and metastatic breast cancer when under treatment.
#22 ProSigna Assay
This is a breast cancer prognosis signature assay earlier known as PAM50. This genomic test undertakes an analysis of genes in early stages of hormone receptor + types of cancer of the breast. This test should be used for making treatment decisions based on the chances of cancer returning to different parts of the body within 10 years of diagnosis for women post-menopause and hormone receptor-positive breast cancer with three positive lymph nodes post hormonal therapy for 5 years. This test was approved by US FDA in 2013 and received the CE EU approval mark in 2012.
#23 Subtraction Probe Technology
SPoT-Light HER2-CISH stands for Subtraction-Probe-Technology-Chromogenic- In-Situ-Hybridization. This is a test to check if the breast cancer linked cells are HER2 +, as these have receptor proteins which are excessive in number at the cell surface. Receptors receive signals outside the cell, ensuring growth and division. This CISH test was approved by US FDA in the year 2008. It can detect HER2 genes in the breast cancer tissue sample.
#24 Thermography
This is also known as thermal imaging and uses a special camera for measuring the degree of temperature on the breast surface. This test is non-invasive and involves zero radiation. As cancer cells grow and replicate super fast, blood flow and metabolism remain higher in cancerous tumors. Skin temperature goes up as the blood flow and metabolism rise.
#25 Ultrasound
This is an imaging test sending high-frequency sound waves to the breast and converting them to screen images. The ultrasound requires the positioning of a sound-emitting probe on the breast for conducting the test. No additional radiation is involved. Ultrasounds are not used as screening tests for breast cancer. It works instead to act as a complementary test for other screening tests. In case the pathology is not detected by physical exam or mammography, the best way to find out if it is a solid or fluid-filled growth is through ultrasound. For those under age 30, the doctor recommends ultrasound prior to mammography for evaluation of the breast lumps. Breast lumps can be tough to detect for those under age 30, so medical assessors and doctors may suggest ultrasound even before mammography. Mammograms are harder to carry out in younger women as their breasts are denser. Ultrasound can also be used for guiding biopsy needles to certain areas in the breast.
#26 Urokinase
The proteins in the external part of the tumor cells that spur growth are urokinase plasminogen activator and its inhibitor. Testing for the proteins is carried out on breast cancer tissue at the time of surgery or biopsy. Women with HER2 negative, hormone receptor-positive breast cancers which are node negative can be diagnosed through the urokinase test. Cancer having these characteristics is considered less likely to recur. Cancers with these characteristics offer low recurrence risk and knowing these two protein levels ensures that chemotherapy or other treatments post surgery can be carried out.
Treatment
Photo by: Kabusa16/CC BYFor treating breast cancer, a multidisciplinary team is assigned to work together and provide exceptional care and treatment. Main breast cancer treatments are surgery, chemotherapy, radiotherapy, hormone, and biological therapy. One can either opt for these treatments or a combination of these. The treatment type is associated with the diagnosis of cancer and the stage at which it is detected. Breast cancer diagnosed can be at an early stage. If breast cancer is diagnosed at an advanced stage, different treatment is required. The healthcare team will find out which treatments are most suitable. Choosing the right treatment involves considering the cancer grade and stage, general health and whether menopause has been experienced (the latter for women patients only). The treatment needs to be discussed with the care team as well.
Most breast cancer types are detected in earlier stages. Some proportion of women also discover breast cancer at the advanced stage. Secondary or metastatic breast cancer is not curable. Treatment is therefore focused on attaining remission for cancer patients, where cancer shrinks or is eliminated.
#1 Surgery
Surgery is the first treatment type for breast cancer. The nature of the surgery undergone depends on the breast cancer type. Surgery is generally supplemented by chemotherapy/hormone or biological treatments/radiotherapy. The treatment depends on the nature of breast cancer. The most suitable treatment plan can be considered.
Two main types of breast cancer surgery are breast conserving and mastectomy. In breast-conserving surgery, cancerous lumps are removed. Surgery can be used to remove the entire breast in a mastectomy. Post the mastectomy, the reconstructive surgery can be used to replace the removed breast. Breast-conserving surgery post radiotherapy is important as total mastectomy for managing early-stage breast cancer disease.
Breast Conserving
Breast-conserving surgery ranges across a wide spectrum from lumpectomy to wide local excision. In this case, the tumor and the surrounding breast tissue is removed to quadrantectomy or partial mastectomy, where a quarter or one-fourth of the breast is operated on. If one has breast-conserving surgery, the breast tissue removed depends on the nature of cancer, the type of tumor and its location in the breast and amount of surrounding tissues that can be eliminated. The size of the breasts is also a deciding factor.
The surgeon will remove an area of healthy breast tissue around cancer, tested for traces of the disease. In case cancer is not present in healthy tissues, there’s less likelihood of cancer return. In case cancer cells are found in adjacent tissues, more tissue needs to be removed from the breast. Post breast-conserving surgery, radiotherapy is needed for destroying additional cancer cells.
Mastectomy
This is surgery which involves the removal of the entire breast tissue, including the nipple. As no obvious signs are there cancer has reached lymph nodes, the mastectomy will be carried out where the breast is removed with sentinel lymph node biopsy.
If cancer has spread to the lymph nodes, the extensive removal of these nodes from the axilla under the arm is essential. Breast reconstruction is then following the mastectomy, where a new breast shape looking like the removed breast is carried out. It can be immediate or delayed reconstruction. This can be carried out by inserting breast implants or using tissue from another body part to form a new breast.
Lymph Node Surgery
In case cancer has spread, the procedure is known as sentinel lymph node biopsy. These are the first lymph nodes that cancer cells reach if spread. These are part of the lymph nodes that are reached by cancer cells post metastasis. Part of the lymph nodes is under the arm. These are the axillary lymph nodes. The sentinel lymph node positioning varies, so it is identified using a combination of radioisotope and blue dye. Sentinel lymph nodes are examined under the lab to check if the cancer cells are there. This indicates if cancer has spread. If more cancer cells aggregate in the sentinel nodes, further surgery may be needed.
#2 Radiotherapy
Radiotherapy uses controlled radiation doses to kill cancer cells. This is post surgery and chemo to kill remaining cancerous cells. If one needs radiotherapy, the treatment commences a month post the surgery or chemo, so recovery is facilitated. Radiotherapy sessions last 3-5 days in a week for 3-6 weeks for a few minutes.
The kind of radiotherapy depends on cancer and the surgery type. Certain women may not need radiotherapy at all.
Breast radiotherapy takes place post breast-conserving surgery. Radiation is also applied to the entire remaining breast tissue. In chest wall radiotherapy, radiotherapy is applied to the chest wall post the mastectomy. Women undergoing radiotherapy may receive a boost of it. Lymph node radiotherapy is aimed at the armpit or axilla and the area around it to destroy the cancer present in the lymph nodes. Side effects of radiotherapy include darkening and skin irritation, sore, redness of the skin, extreme fatigue and more fluid build up in the arm caused by lymphoedema.
#3 Chemotherapy
This involves the use of cytotoxic or anti-cancer medication for destroying cancer cells. It may be used post surgery to remove cancer cells which still remain, in which case the adjuvant chemotherapy is applied. In certain cases, chemotherapy may take place post the surgery to cut down a big sized tumor in which case it is neo-adjuvant chemo. Numerous medicines are employed for chemotherapy and these are given at one go. Choice of combination and medicines will depend on type and spread of the breast cancer.
Chemotherapy is provided as outpatient treatment. The medicines are applied through a drip via the vein into the blood. Certain patients may even be provided tablets that can be taken at home. Chemo sessions may take place once every 2-3 weeks across a duration of 4-8 months to provide the body rest between the treatments. Main side-effects of chemo result from the influence on healthy, normal cells impacting immunity.
Side effects range from loss of hunger, infections, nausea and puking, fatigue, hair loss and soreness of the mouth. Side effects may be controlled or prevented with medicines prescribed by doctors. Chemo medication also halts the estrogen production in the body, encouraging the growth of certain breast cancer cells.
In case one has not experienced menopause, the periods may cease while undergoing chemotherapy treatment. Once the duration of chemo is over, ovaries start producing estrogen again. This may not always take place and early menopause may be entered. This is even likelier so in those over 40, as one reaches near the menopausal age. The impact the treatment will exert on fertility is important.
Chemo for secondary or advanced breast cancer cannot cure the disease. But it can shrink the tumor, leading to symptom relief and lengthen the life.
Chemotherapy is the utilization of drugs to eliminate cancer cells and prevent the ability of the cells to replicate and grow. Systemic chemo reaches cancer cells throughout the body. Easy ways to provide chemotherapy include IV tubes placed into the vein through a needle, a subcutaneous injection under the skin or the intramuscular injection. Oral pills and capsules are also considered.
Chemo must be provided prior to surgery to shrink a large tumor and make surgery easy or reduce the risk of recurring. Common drugs for chemotherapy include Ixempra, Halaven, Navelbine, Abraxane, Taxol, Methotrexate, Adricul, Ellece, Doxil, Adriamycin, Taxotere, Dcoefrez, Neosar, Platinol, Paraplatin, and Xeloda. A patient may receive a single drug or combinations at different times. Studies show that combinations are more effective for locally advanced breast cancer and early-stage cancer. The combinations are as follows.
AC comprises cyclophosphamide and doxorubicin. AC or EC is epirubicin plus cyclophosphamide and T or doxorubicin and cyclophosphamide followed by docetaxel and paclitaxel or the opposite. CAF is cyclophosphamide, 5-FU, and doxorubicin. CMF stands for cyclophosphamide, methotrexate, and 5-FU. TAC stands for docetaxel, cyclophosphamide, and doxorubicin. Docetaxel and cyclophosphamide or TC also work well.
Therapies that specifically work for the HER2 receptor may be provided with chemo for HER2 positive breast cancer. Side effects of chemo depend on the drugs used, individual and the dosage and schedule of drug used. Side effects include tiredness, infection risk, hair loss, vomiting and nausea, appetite loss and diarrhea. Side effects can often result after post medications and can go away once treatment is over. Long-term side effects may also take places such as nerve, heart damage or secondary cancers. During chemo, remaining healthy is the main focus.
Additionally, bone-modifying drugs block the destruction of the bone and help to strengthen it. These are important for preventing cancer from recurring in the bone or treating cancer that has metastasized to the bone. Specific types are also used in low dosages to treat bone thinning or osteoporosis. Bone destruction blocking drugs used for breast cancer patients include bisphosphonates and denosumab.
#4 Hormone Treatment
Certain breast cancers receive stimulation from naturally occurring hormones found in the body such as estrogen and progesterone. These type of cancers are called hormone receptor + cancers. Hormone therapies lower the hormones in the body or stop their impact. This hormone therapy is based on grade and stage of cancer, the hormone it is responsive to, the age, whether menopause has been experienced and the nature of treatment one is undergoing. Hormone therapy post surgery and chemo is not always the norm. Sometimes, it is provided prior to the surgery for shrinking the tumor, making it convenient for removal. Hormone therapy remains the go-to treatment for breast cancer if general health prevents surgery, chemo or radiation therapy. For different cases, hormone therapy is taken for five years post surgery. If the breast cancer cells are not sensitive to the hormones, the therapies will have zero effect.
#5 Biological/Targeted Therapy
Specific breast cancer types are the result of a protein referred to as human-epidermal-growth-factor-receptor/HER2. Such cancers are known as HER2+. Biological therapies work through the stoppage of the impact of HER2 and help the body’s immunity to fend off cancer cell growth. If there are massive levels of the HER2 protein and one has biological therapy, medications like trastuzumab may be prescribed.Also called Herceptin, it is used once the chemotherapy is over. Antibodies take place naturally in the body and are created to destroy cells such as bacteria and viruses from the immunity. This antibody targets and eliminates HER2 positive cancer cells. Trastuzumab is provided through an intravenous drip. It can be injected beneath the skin or subcutaneously. Each treatment session takes close to 60 minutes. Amount of sessions depend on the degree of advancement of breast cancer. On an average, a session is needed once every 3 weeks for early stage breast cancer and if the cancer is advanced, weekly sessions are required.This can also lead to side effects such as heart issues. If you suffer from cardiovascular problems such as angina high blood pressure or heart valve illness, regular tests need to be taken to prevent complications.
Clinical Trial
A lot of progress had resulted in treatment and women live longer with lesser side effects. The discoveries in clinical trials ensure new treatments or combinations are compared with standardized ones. Participants in clinical trials can benefit from the care. If one is required to be in a trial, the information sheet is provided and the consent form needs to be signed. Refusal or withdrawal from clinical trials without impacting care can be a real problem.
#6 Psychological Counseling
Combating cancer is a massive challenge for patients and their loved ones. It leads to emotional and real problems. Women have to endure the removal of part or whole of a breast affected by the disease. It is important to discuss feelings and difficulties with therapists and trained counselors. Help can be taken at different stages of the illness. Numerous ways are there to find support and help. Hospital doctors, specialist nurses or GPs can refer one to the counselor. If one is depressed, approaching the GP and specialists is better as antidepressant drugs can help. Psychologists and counselors can also lend a helping hand. Numerous organizations have online forums and helplines. This connects you with those who have had treatment.
#7 Complementary Therapies
These are holistic, comprehensive therapies promoting physiological and emotional well being. They are provided along with more conventional treatments like relaxation techniques, aromatherapy, massage, and acupuncture. Women can cope with diagnosis and therapy/treatment, providing a break from the plan. Complementary therapies need to work in conjunction with conventional treatment.
Treatment As Per Stage
Numerous ways are there to treat cancer, based on the stage and type. Local treatments offer a cure for the tumor without impacting the rest of the body. This includes surgery and radiation therapy. Drugs are used to reach cancer cells and offer systemic treatment. They can be taken orally or injected into the bloodstream, based on the type of cancer. Medicines and drug treatments include chemo, targeted therapy, and hormone therapy. More women opt for more than one type of treatment for cancer. Many women with breast cancer have a certain type of surgery for removing the tumor. Based on how aggravated the stage is and the nature of breast cancer, other types of treatments can impact treatment pre or post surgery or during both stages.
Treatment plans involve the services of breast oncologist or breast cancer surgeon for treating cancer, radiation oncologist, medical oncologist, and plastic surgeon. The surgical oncologist employs surgery to cure breast cancer. Chemo is provided by the medical oncologist while the radiation oncologist provides radiotherapy. Plastic surgeons repair different parts of the body.
Goals and possible side effects need to be considered, and the decision that makes for the best fit is essential. The behavior and biology of breast cancer impact the treatment plan. While some tumors are smaller, others are larger and the rate of growth varies. Treatment options are personalized and are based on numerous factors such as tumor subtype, tumor stage, genomic markers, patient age, health, preferences and menopausal status. Presence of known mutations in breast cancer genes can also be implicated in the etiology of this disease.
While the breast cancer care team members tailor treatments for patients and breast cancer, early stage, as well as locally advanced breast cancer, needs to be considered.
Early Stage Cancer
For early-stage invasive breast cancer and DCIS, doctors need to remove the tumor. For cancers that are larger or growing more quickly, systemic treatment with chemotherapy or hormonal therapy known as neoadjuvant therapy works well. Post the surgery, the risk of recurring needs to be lowered and the aim should be to remove remaining cancer cells. These cancer cells are responsible for recurrence as growth occurs across time. Treatment post surgery is known as adjuvant therapy. This includes radiation, chemotherapy, targeted therapy, and hormonal therapy. While adjuvant therapy depends on the chance that cancer cells in the breast or body and the possibility that specific treatments can work to cure cancer. Adjuvant therapy lowers recurrence but it is not devoid of risk.
Apart from staging, other tools can be used for estimating prognosis and doctors can make important decisions about adjuvant therapies. Tests need to predict recurrence risk by testing tumor tissues. These tests help doctors to better understand risks from cancer and if chemotherapy can lower risks. Surgery for removing the cancer is not possible in some cases, which are inoperable. The doctor then approaches treatment in a different way. Chemo, hormonal therapy, radiation therapy or targeted therapy can work well. For cancer that is recurrent, treatment options depend on the way the treatment took place, and the nature of cancer such as HER2, ER, and PR.
The most common options for early and locally advanced breast cancer are as follows. The care plan should include treatment for side effects and symptoms. Learning about all treatment options are a must. Questions need to be asked about factors that are unclear. The goals of treatment and what can be expected in return are important. Those who are 65+ can opt for geriatric assessment before treatment planning.
Systemic treatments like chemo work well for younger and older patients alike, but senior patients may experience more side effects. For example, breast cancer drug trastuzumab can cause heart problems. This is more so for patients with heart disease who receive a combination of chemo. Patients need to consult with the doctor regarding systemic options and study risks and benefits. Potential side effects, as well as their management, is important.
For people of different ages, cancer and the treatment can exacerbate side effects and symptoms. For treatment that stops, slows or removes cancer, side effects and relief are also essential. Palliative or supportive care provides the help needed to physically, emotionally and socially support the patient.
Palliative care is treatment focused on lowering symptoms, enhancing the quality of life and providing supportive care for patients and their families. People, irrespective of age or stage of cancer, can opt for this care. Palliative care needs to commence early in the treatment process. Less severity of symptoms, better quality of life and greater levels of satisfaction with the treatment are reported. Palliative treatments vary and include relaxation methods, emotional support, nutritional support, medications, and other therapies. Chemo, surgery or radiation therapy should also accompany this. Before treatment, health care practitioners need to have a frank discussion with the patient to understand possible side effects.
Recurrent Breast Cancer Treatment
In case cancer does not come back after early-stage disease, it is known as recurrent cancer. When the breast cancer recurs, it can come back in different parts of the body such as original cancer (known as local recurrence), chest wall or lymph nodes under the chest or arm known as regional recurrence. Other places include distant organs like brain, liver, lungs, and bones. Distant or metastatic recurrence can be tough to treat. When breast cancer recurs, a fresh cycle of tests is needed to guard against recurrence. Imaging tests may also be included along with biopsies to confirm breast cancer recurrence. Post the tests, the doctor will consider treatment choices in consultation with the patient. Treatment plans include those described such as radiation therapy, surgery, hormonal therapy, targeted therapy, and chemotherapy. This can be used in various combinations or varied paces. Treatment options for recurring breast cancer are based on previous treatment for the original disease. Time elapsed since initial diagnosis and recurrence location are also considered. The PR, ER and HER2 status of the tumor need to be considered as well.
Those with recurrent breast cancer experience problems like fear or disbelief. Talking with the health care team about support services is important, as well as learning how to deal with a recurrence of the disease. Local or regional recurrence is managed and curable. Treatment options include mastectomy for recurrence. Cancer is completely eliminated through this method. For those with region or location-based recurrence in the chest wall post the mastectomy, surgical treatment is followed by radiation therapy to the affected area. If radiation therapy has been provided for initial cancer, this is not an option. Radiation therapy is provided at the complete dose in the same area at more than one point in time. Other methods to reduce distant recurrence include chemotherapy, radiation therapy, hormonal therapy, and targeted therapy. This depends on the tumor and the kind of treatment earlier received. Regardless of which treatment plan is chosen, palliative care can play an important role in symptom relief and alleviation of side effects. Clinical trials may also be helpful for those looking to deal with multiple bouts of cancer.
Treatment in Stages 1-3
When it comes to treatment, the stage or extent of the breast cancer is a crucial factor in deciding about treatment. Many women with stages 1-3 of breast cancer are offered treatment with surgery and radiation therapy post operation. Some kind of drug therapies may also be used. The wider the spread of cancer, the greater treatment one requires. Treatment choices are impacted by requirements and preferences and cancer-related data like whether it is ER, PR or HER2 positive, the extent to which cancer growth is there as measured by grade/stage. The health of the patient is also an important consideration. Postmenopausal women will have different treatment options as opposed to those who have yet to undergo it.
Women in stages 1-3 may also be treated with chemotherapy, hormone therapies involving tamoxifen and aromatase inhibitor or both. HER2 drugs like pertuzumab and trastuzumab may also be considered along with a blend of these. The kind of drugs that work best on the hormone receptor status and other factors also come into play.
Stage 1 cancer is generally small in impact and has not reached the lymph nodes or just a small area of the sentinel lymph nodes. Surgery forms the key treatment for breast cancer at stage 1. Cancers are also treated with breast- conserving surgery called lumpectomy and/or partial mastectomy and all lymph nodes including the sentinel and the axillary need to be checked out. In some instances, breast reconstruction surgeries can be carried out for cancer treatment. If radiation therapy is required, it may be done prior to the reconstruction. Hormone or chemotherapy may be required depending on whether breast cancer involves ER, PR or HER2+ cancers.
Stage 2 cancer is treated with breast-conserving surgical procedures and mastectomy. The closer lymph nodes will be checked with the sentinel or axillary dissection of lymph nodes. Women with breast-conserving surgery also undergo radiation while those with mastectomy can undergo it if the cancer is detected in lymph nodes. If one is first diagnosed with stage 2 breast cancer, and treatments like hormone therapy or chemotherapy prior to surgery, radiotherapy is recommended in case the cancer is detected in the lymph nodes during the mastectomy. Those specializing in radiation such as radiation oncologists may also review the case. Chemo may also be needed. Additionally, adjuvant and neoadjuvant systemic therapy is prescribed for those with stage 2 breast cancer. Drugs are based on the age and hormone receptor as well as the status of the tumor. Chemotherapy may be administered pre or post surgery. In case HER2 positive cancer is detected, targeted therapy may also be included. If the cancer is ER or PR+, hormone therapy may be tried.
Stage 3 breast cancer has tumors which are more than 5 cms/2 inches in width. These also may grow into the close area by tissues such as the skin above the breast or the muscles underneath. Cancer may also have spread to an additional lymph node. If there are inflammatory breast cancers, the treatment will take a different direction. Cancer is managed with neoadjuvant chemo prior to surgery, shrinking the tumor to permit partial mastectomy or complete mastectomy depending on the case. The lymph nodes nearby also need to be monitored. Sentinel lymph node biopsies don’t work for stage 3 cancers, so ALND may be carried out for axillary lymph nodes.
Radiotherapy is also required post-surgery. In case breast reconstruction surgery is carried out, it is delayed post the completion of the radiation. In certain cases, adjuvant chemotherapy is given post the surgery too. Women with HER2+cancers are administered trastuzumab post the surgery to complete the treatment taken with the drug. Those with hormone-receptor + breast cancers can also opt for adjuvant therapy.
Treatment with surgery may be yet another choice for those with stage 3 cancers. Surgery may be followed by chemo or hormone therapy, depending on the nature of breast cancer.
Treatment of Stage 4 Cancer
Women with stage 4 or advanced cancer can opt for systemic therapy, including hormone, chemo, targeted therapy or a blend of these. Localized treatment options like radiation or surgery may also be used to prevent or cure symptoms. Stage 4 cancers also spread to the breast and nearby lymph nodes as well as other parts of the body such as the liver, lungs, and bones. It may also extend to the brain or several other organs.
For those with stage 4 breast cancer, systemic treatments are the best means to manage symptoms. Treatment may shrink the tumor, slow down the cancer growth and improve symptoms to enable women to live longer. These are considered incurable cancers. Type of drugs used for stage 4 breast cancer depends on hormone receptor status and HER2 status of cancer.
While systemic drug treatment is the main treatment option for metastasized cancer, local as well as regional methods of treatment like partial chemo, surgery or radiation therapy are used as well. Radiation therapy and surgery are used when there is an open wound in the chest or breast, and treatment of smaller metastases in specific areas like the brain. Radiation therapy may also be employed to avert fractures, and check the area of cancer spreading on the spinal cord. Treating blood vessels blocking the liver or providing relief of pain or additional symptoms is important. Regional chemotherapy is when drugs are injected into a specific area like the fluid surrounding the spinal cord and the brain.
Treatment: Summary
Treatment for relieving symptoms is based on the nature of the metastases. Pain from bone based metastases can be treated using radiation therapy, drugs like Zometa or Aredia and Zgeva. For advanced breast cancer, treatment can shrink cancer or slow down its growth. After a while, it tends to cease working. Treatment efficacy depends on factors like previous treatments, the area where the cancer is located and the age, general health as well as treatment orientation of the patient. If cancer ceases to respond to one form of chemo, another may be opted for.
Recovery
There are a lot of guidelines for breast cancer surgery recovery. The specific instructions post the surgery or treatment must be followed.
#1 Drainage
Post the surgery, one is discharged from the hospital with an external device for drainage in place. The drains remove and collect fluid from the site of the surgery. Measuring fluids, emptying the drains and keeping a watch on issues is a must during the stage. The nature of fluid that drains decreases eventually changing in color once the process is over from red to straw shades. Drainage is removed 1-3 weeks post surgery.
#2 Bandages
For women, a special inner wear is provided to hold bandages in place post the surgery. The bra may be removed and changing the dressings from the surgery is an important factor here. Incision needs to keep dry and clean for 1-week post the surgery, with sponge baths rather than showers. Incision areas must be kept dry while bathing. The tape over the incision eventually falls off on its own.
#3 Skin Care
The skin may appear dark and damaged post breast cancer operation. This lasts for only a few days. There may be numbness or discomfort and tingling in upper limbs and this will dissipate with time. While shaving beneath the arms or applying deodorant, incisions should be avoided by checking the look in the mirror. Once it heals, the thick, tough incision can soften and smoothen. Use vitamin E, pure lanolin or mild lotion rather than lotions with fragrances that can prove irritating to the skin.
#4 Pain Medication
A prescription for pain medication post breast cancer surgery is important. OTC pain relievers along with prescription pain medication need to be taken. Don’t opt for aspirin or other products containing this medicine for the first three days post the procedure. This can cause bleeding.
#5 Exercises Post Surgery
Everyday stretching exercises can help in regaining mobility yet talking to the surgeon about when to commence with this is important. While seated or standing at the chair’s edge, both arms need to be lifted over the head with the elbows close to the ears. This is held for 5 counts and then repeated.
Arm swings are also a good way to strengthen your body post the surgery. Swinging arms like a pendulum, the elbows need to be kept straight. The distance of the swing needs to be raised each time. Do 10 repetitions.
#6 Follow Ups
Additional follow-up visits are essential post the breast cancer surgery/chemo or radiation therapy. Cancer should be in remission and not recur. The checkups include chest, underarm and neck exams. Across time, one can get a complete yearly mammogram and physical. Additionally, no blood tests, scans or X-rays need to be carried out on a regular basis.
Doctors need to be informed in case a person recovering from breast cancer treatment feels a loss of hunger or loses weight. Changes in menstruation patterns, blurring of vision, coughing, hoarseness or dizziness and shortness of breath, as well as headaches and chronic digestive problems, need to be looked into as well.
Survival Rates
Survival rates inform the extent to which people are alive and well with a certain period of time for a specific type and stage of cancer. This does not indicate how long one will live but gives an understanding of the treatment success rate. Statistics on the outlook for certain stages and types of cancer are often provided as 5-year survival rates. Many live longer than this. A 5-year survival rate of 80 percent means 80 of 100 patients who had this cancer are alive post diagnosis within a period of 5 years.
Relative rates of survival are more accurate for estimating the impact of cancer on surviving. These compare those who have breast cancer with women in the total population. If the five-year relative survival rate for cancer of a certain category is 70 percent, it means those who have cancer are 70 percent as likely to live for a period of a minimum of 5 years post-diagnosis. The five-year relative survival rate is an estimate and outlooks can vary based on a whole load of factors.
Survival rates are associated with the previous outcomes of a massive number of persons who had the disease, but the particular patient’s case cannot be specifically predicted. The five-year relative survival rate for women with stage 0 or 1 breast cancer is around 100 percent. For those with stage 2 breast cancer, the five-year relative survival rate is 93 percent. For those with stage 3 cancer, the rate is 72% while for those with stage 4 cancer, the rate is 22%.
Survival rates are estimates, but they cannot predict what will happen. Difficult emotions may be felt when people realize the cancer is receding. Along with anxiety, there is fear, insecurity, sadness, and depression apart from guilt, anger, embarrassment and loss of confidence. Strong emotions are felt post the cancer treatment. Oncologists and other members of the care team can guide you to proper counseling and therapy.
Fear of recurrence is one of the biggest hurdles in the recovery process. Prior to follow-ups, if possible symptoms are noted, worries will diminish as time progresses. A way to deal with the anxiety is to have a clear follow-up plan and with recurrence, early detection is the step forward if symptoms are noted.
Symptoms you need to watch out for are changes in the treated or untreated breast. Additionally, unexplained pain also needs to be taken into account. Weight changes or loss of appetite, vaginal bleeding or changes in menstruation need to be heeded, as do coughing, hoarseness, and backaches.
Rehabilitation
Breast cancer treatment can impact functionality and energy levels. Many breast cancer treatment and therapies lower estrogen in the body, leading to reduced bone density. Exercising can be used to promote bone density and lower the risk of recurrence of breast cancer. Exercise can also ward off treatment based fatigue. The oncology rehab team helps patients to overcome the loss of strength and tiredness and reduce pain. Oncology rehabilitation therapists can work with surgical oncologists to prevent or lower lymphedema through the use of massages, stretching exercises, and drainage methods. Scar and myofascial massage post surgery can lower discomfort and pain. Neuromuscular training and therapy can create energy and strength to participate in activities that are of importance. Ariculotherapy can alleviate breast cancer treatment like fatigue, nausea and pain. Rehab therapists can work with the treatment group to improve physical functioning and well being. The rehab team provides the ability to understand the physiological and psychological payoffs of restoration.
Oncology rehab includes numerous therapies for building endurance and strength, regaining independence and reducing stress as well as maintaining the endurance to take part in everyday activities of critical importance to patients. Physical therapies are needed to provide ranges of motion training and exercises that utilize light resistance. These exercise lower fatigue and enhance physical function, well being and safety. Occupational therapists can assist with everyday living activities of importance to the routine and life quality such as eating, dressing, and showering. Many cancer sufferers also undergo speech or language deficits, on account of problems in swallowing, dryness of the mouth, loss of voice and brain changes which are the outcome of cancer treatment. Additionally, massage therapists reduce the pain and enhance the quality of life for cancer patients. Traditional massage aside, there’s stone therapy, soft tissue manipulation with passive stretching, myofascial release, aromatherapy, trigger point therapy, effleurage massage, friction, reflexology, and acupressure.
Chiropractors perform sessions to relieve pain without any medicine or surgery. This can help to alleviate pain and nausea. Noninvasive auriculotherapy is a form of cancer rehab that alleviates breast cancer side effects by stimulating the auricles of the ear. Lymphedema is the collection of fluid in tissues leading to swelling. Various surgeries for breast cancer can trigger this and rehab teams provide assistance about how to reduce swelling, especially through the use of surgical options.
Preventative, supportive, restorative and palliative interventions are essential for ensuring successful rehab. Once the condition of the patient stabilizes, rehab therapists need to provide home based care to prevent reconditioning. Late-onset impact of cancer and its treatment or therapy include cognitive defects, inactivity, pulmonary disease, obesity, pain, diabetes and cardiovascular diseases.
Quality of life is an important consideration for patients undergoing rehab post their cancer. Rehab programs include fitness and sports activities, relaxation therapies, patient education, counseling and socio-cultural as well as dietary support. Dealing with problems like neuropathy, swelling of the limbs due to fluids and pain can be major goals during rehab for cancer patients. Want to learn more about breast cancer , visit www.bookinghealth.com .
Conclusion
Breast cancer is a chronic disease. But management and treatment can make for a better prognosis and lead to recovery. The care your medical practitioners provide can be life giving and patients need to maintain a positive mindset for better survival rates and faster recovery, lack of recurrence and the elimination of symptoms.

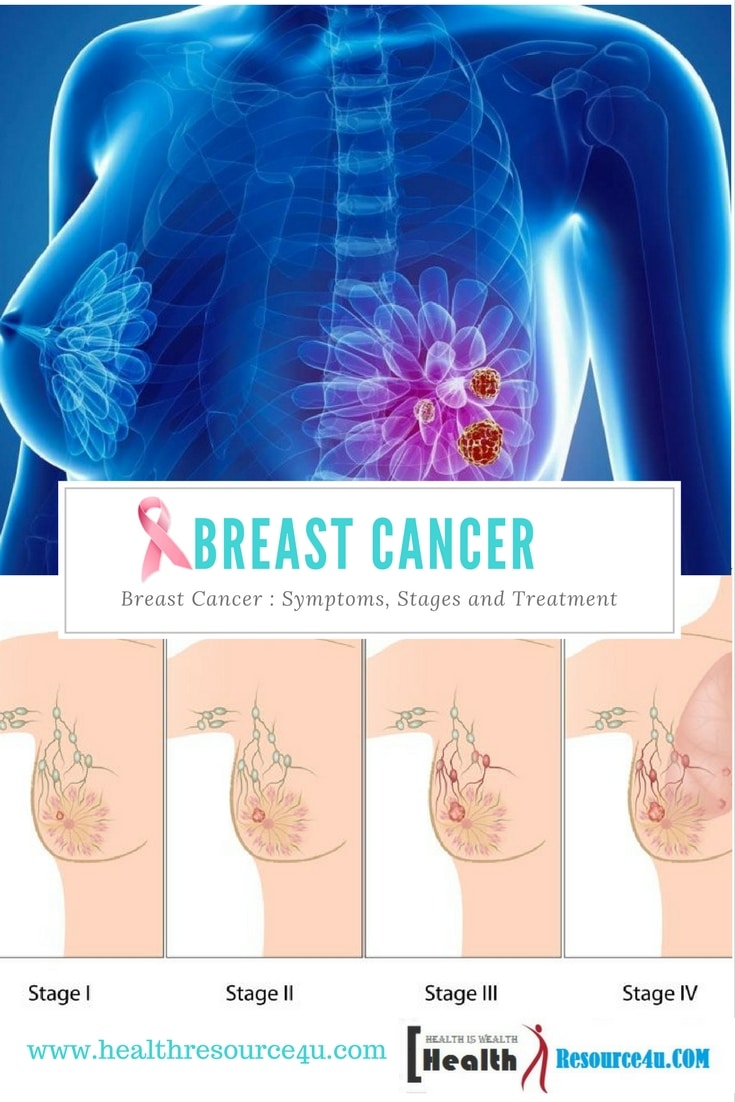
Hi, Janhvi Johorey
Thanks for your nice explanation. After skin cancer, breast cancer is the most common cancer diagnosed in women in the United States.