Female sterilization, also known as tubal sterilization, is a massive decision as it is a final kind of contraceptive. It does not allow women to get pregnant ever again. Adult women without any desire for children or those who don’t want more children, or cannot manage a pregnancy on the basis of medical problems should opt for this contraceptive method. Another choice for irreversible birth control can be sterilization or vasectomy for men.
Learn More About Tubal Ligation
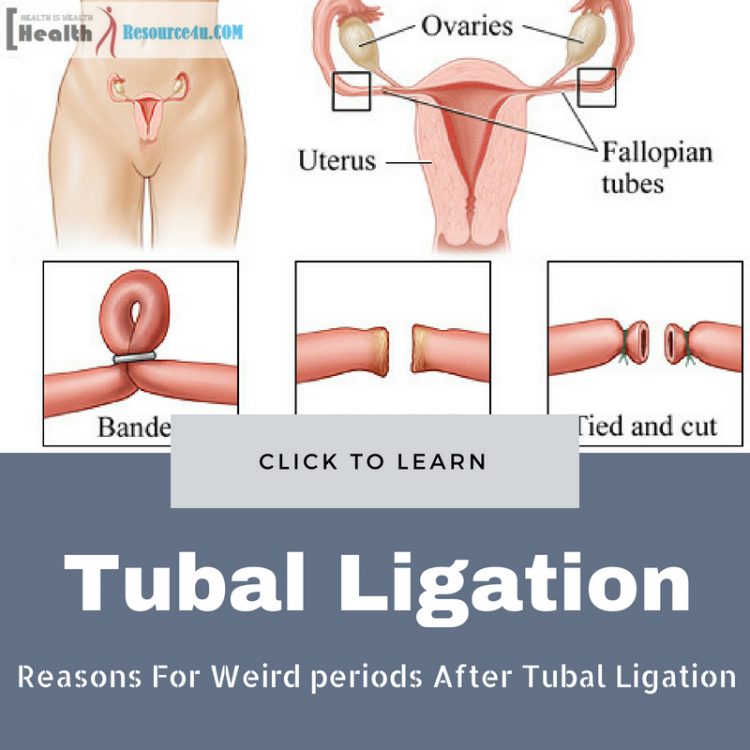
Tubal is associated with a woman’s fallopian tube. Ligation means cutting, closing or tying off. Tubal ligation concerns minor forms of surgery. The fallopian tube is where the sperm and egg fuse to fertilize the egg before it attaches itself to the reproductive system, specifically the uterus. Through the closure of the tubes, sperms cannot reach the egg and this leads to less likelihood of pregnancy. Female sterilization should be performed in an OR or clinic based on the procedure used. It could be carried out while sleeping or awakened. If awakened, one is given anesthetic medicine, so there is no discomfort. Based on the kind of method chosen, one can have a minute incision in the abs or the process can also be carried out vaginally, sans cuts or incisions.
In the laparoscopic sterilizing procedure, a small incision is attempted in the belly, following which a laparoscopy is placed within the belly close to the navel. The fallopian tube transport all the eggs from the ovary into a uterus. The second instrument is then used to close it. The procedure is carried out in an OR under generalized anesthesia while resting at a given time except immediately after a baby is delivered. In this case, fallopian tubes can be cut, tied, removed and stitched with suturing material or burnt. Additionally, fallopian tubes can be completely removed as well.
Sterilizing using the electrical current aims for burning and destroying the fallopian tubes once these tubes have been operated on. Sterilization carried out with electrical change cannot be turned back. Via the laparoscopy, the surgeon inserts a tool that is special and stretches the plastic band, picking up a tiny fallopian tube, and place the plastic band above the loop. The tube is clamped shut. The silicone band is a tube based ring through which the surgeon inserts a special tool stretching the plastic band, picking up the smaller loop of the fallopian tube, and placing the plastic band across the loop. Finally, the tube is further clamped shut then. Spring clips are then used for clamping off tubes. Much like a pin to hold clothes, it is placed above the fallopian tube and can be closed through the spring type clip. The type is a kind of rounded clamp, placed over the fallopian tubes. The plastic liner of the clamp increases keeping the tube shut as it flattens.
Minilaparotomy is a procedure used in an OR with general/local anesthesia within one to two days after a woman has conceived.
Then, there’s hysteroscopic sterilization is known as the Essure technique and is carried out in operation or clinic setting using anesthesia about seven to ten days after the woman’s period. Once the patient awakens, the doctor inserts a thinner camera instrument or laparoscope towards the end, within the vagina, passing through the uterus, cervix and finally the fallopian tubes where a smaller coil is placed. Scarring of tissues takes place and seal the tube closed. As this involves time to take place, another birth control method should be used for the first three months.
The follow-up called Essure Confirmation testing is performed in a period of three months post the procedure. This is akin to an x-ray that causes the doctor to observe tubes that are sealed off. When the tube is effectively sealed at a point, the healthcare provider can tell that other types of birth control methods should be stopped at this point. Essure testing cannot be done during birth.
Complications are very rare and taken from generalized anesthesia, specifically not the procedures. There exists a low chance of damaging the bladder, or even bowel or large blood vessel. For electric currents destroying the fallopian tubes. Presently, there exists a low likelihood of bowel or skin burning or damage to other inner organs. Other issues and side effects include infection and bleeding. The possibility of pregnancy after sterilization is rare. If pregnancy occurs, a woman is likely to have specifically tubal/ ectopic pregnancy which may be really tough.
Following laparoscopic procedures, one will remain in a recovery room unless awakened and can only consume light foods. Most ladies leave the hospital within two to four hour per day. One needs an individual to bring them to a hospital and bring them home, too. Women may experience mild pain and discomfort for some days in some cases. If the symptoms last beyond 2-3 days, call the health care providers. Most can return to work or activity within a week of undergoing the process, yet everyone varies. There can be giddiness, shoulder pain, bloated feelings or cramps.
Before signing the permission for carrying out the procedure, the health care providers need to talk about risks like infection, pelvic discomfort, partial blockage of the tube and the rare chance of exacerbating holes in the uterus and/ or fallopian tube.
When the medicine is given before the procedure for helping one relax and block tubes spasms, the procedure takes 30 to 45 minutes. One can leave for home shortly post the process and tend to normal activities after a day.
How Female Sterilization Works?
Sterilizing women is the ideal birth control method available. It is around 100 percent effective. Female sterilization protects against STIs. Female sterilization procedures do not offer protection against STI/STD, however.
Female sterilization does not impact performance or the ability to engage in intercourse. However, there is a chance that female sterilization may not be impacting your periods in a uniform way.
How Tubal Ligation Impacts Periods
The periods could end up with no impact. Medical research has shown sterilized women may actually have less bleeding during menstruation, light flow and lower intensity of menstrual cramps. Call your healthcare provider, if you face any of the following symptoms:
- Missed/late menstrual periods
- Severe low-belly ache
- Feelings like vomiting and the feeling of throwing up
- Tenderness of the breast
If one wants to change their mind, after the tubes are sealed, one may need to have their tubes rejoined. Reversal of sterilization is a difficult operation and it has a 70% chance of success. Less than one percent of women can opt for rejoining their tubes.
Female sterilization is a very safe option for some women such as young ones with serious medical conditions. It can also work out for women who don’t want any kids or even for the ladies who cannot use other types of contraceptive measures. It is also excellent as a procedure for elderly women who do not seek any more kids. Undergoing sterilization is a tough choice. Make sure you consult your healthcare provider and gynecologist if you are considering sterilization for women. It is important to consider the pitfalls and advantages and have all your questions responded to before taking the final decision. If you opt for sterilization, the type of process followed is based on medical requirements and when you must have it carried out. Certain women are sterilized post a pregnancy or an abortion, while many others opt to undergo sterilization once they have recovered.
The origin of post tubal ligation symptoms can be difficult to understand. The body may have gone haywire post the tying of the tubes. Many women report a wide variety of conditions after tubal ligation. There are numerous gynecologic conditions caused and deserving proper evaluation by the doctor.
Problems that can occur after tubal ligation include women experiencing problems. If women have problems after tubal ligation, they have two complaints — changes in the menstrual pattern of periods or even more painful periods. If one has had a tubal ligation and is experiencing these complaints, you could be suffering from an undiagnosed medical condition. To assess if the underlying medical condition causes the symptoms described, it is helpful to consider the terminology for menstrual disorders.
Medical terminology for changes in the amount of bleeding or frequency with one’s periods is oligomenorrhea, hypomenorrhea, and hypermenorrhea or menorrhagia. Menstrual periods that are irregular or infrequent are called oligomenorrhea. Periods that are scarce in terms of bleeding are known as hypomenorrhea. Periods which are heavier and are associated with the higher amount of bleeding are called menorrhagia or hypermenorrhea, both of these are referred to as heavier periods.
The medical terminology for painful periods is dysmenorrhea. Dysmenorrhea is divided into two categories namely primary since puberty, or secondary as one becomes older. More painful periods after tubal ligation are categorized as secondary dysmenorrhea. Medical causes of menstrual disorders including oligomenorrhea, hypermenorrhea or hypomenorrhea range across the following:
- Endometrial polyps
- Uterine fibroids
- Adenomyosis
- Uterine infections
- Endometrial hyperplasia
- Thyroid abnormalities
- Blood abnormalities
- Endometrial cancer
- Ovulation disorders
- Polycystic Ovarian Syndrome
- Pregnancy
- Anorexia nervosa
- Perimenopause
- Pituitary abnormalities
- Congenital adrenal hyperplasia
Most women develop abnormalities in the menstrual cycle post a tubal ligation will not have a serious medical condition. Most come with hormonal abnormalities, uterine fibroids, or anovulation as the cause for changes in the menstrual cycle. Common conditions occur as a person ages or experiences significant changes in weight.
Dysmenorrhea
There are many causes of dysmenorrhea. These are the major causes of secondary dysmenorrhea:
- Ovarian cysts
- Gynecologic disorders
- Endometriosis
- Pelvic Adhesions
- Uterine polyps
- PID
- Congenital obstructive Mullerian malformations
- Cervical stenosis
- Non-gynecologic disorders
- Inflammatory bowel disease
- Irritable bowel syndrome
- Psychogenic disorders
- Uteropelvic junction obstruction
Secondary dysmenorrhea can be felt by many ladies. The most common causes are endometriosis, ovarian cysts, and adenomyosis. It can be difficult to identify the causes of secondary dysmenorrhea. Women may refer to other medical specialists for diagnosing the causes of secondary dysmenorrhea.
Changes in menstrual cycles are common and can impact a tubal ligation. When a woman has a tubal ligation and develops any of the symptoms discussed, it could be the result of post tubal ligation syndrome. The tubal ligation reversal experts recommend seeing a medical provider if there is the development of symptoms post a tubal ligation. The purpose of the visit is to diagnose any medical conditions causing the symptoms. If the doctor is unable to determine medical explanations or symptoms are most extensive than those listed above, this can be attributed to depression, PTSD, anxiety or surgical sterilization issues.
When considering a thorough medical evaluation, there are underlying causes or diagnoses for conditions. The question regarding post tubal ligation syndrome is whether the symptoms develop after tubal ligation are attributable to tubal ligation itself or some other underlying condition? If no underlying causes are discovered, it may be then attributable to tubal ligation.
Tubal ligation, which involves getting your tubes tied, is a common procedure most women have done when they are positive they don’t want more kids. Tubal ligation is a surgical procedure in which the fallopian tubes of women are blocked, cut or tied. This is pretty cut and dry and there may be more to it than one thinks. The more time passes after tying one’s tube, the greater are the chances of pregnancy. According to WebMD, this can be in 5 of 1000 women after the first year and 13 out of 1,000 women after 5 years post tubal ligation.
What increases the chances of becoming pregnant when it comes to posting tubal ligation? The most common reason is that a woman becomes pregnant after tubal ligation when her fallopian tubes grow back or a new passage firms. This lets the sperm meet a released egg. This can cause ectopic pregnancy. In the rare chance of women getting pregnant after tube ligation procedures, the chances of ectopic pregnancy are 25 to 50 percent.
Age plays a factor in the chance of pregnancy after the tubal ligation. Women who are 28 years or younger have a 5 percent chance of getting pregnant after the surgery. Women between the ages of 28 and 33 have a 2 percent chance of pregnancy and there is one percent chance if you are 34 or more. The procedure can be undone, but it is expensive and costly.
Prior to the tubal ligation reversal, it may be an excellent idea to check for possible scenarios that hinder one from becoming pregnant. If there are no complications, then the doctor will need to study your insides. The doctor will insert a light through the belly button to study everything, including fallopian tubes, to check if reversal surgery is possible. If the decisions are made that one are able to have the procedure done, the doctor will make a cut near the area where the cesarean cut is to be made. The surgeon will then disconnect any instrument used to block tubal rings or clips. If there is tubal coagulation one will be able to reattach the fallopian tubes to the uterus through stitches. As the cost of tube reversal is so pricey, couples often decide against the procedure based on this factor.
Ligation means the surgical process of tying an anatomical channel. However, it does result in ovulation and a period every month. Post the tubal ligation, there is no use for ovulation or menstrual periods. While women will have a period after the procedure, some women have claimed their periods are not only much heavier, but obvious cramping can be felt ovulation. Both of these are very real possibilities. Every woman is different and challenges may not be experienced at all. Bodies are unique and so are varying operations and surgeries.
Tubal ligations are easily performed post a C-section. One can also have the tubal done after giving birth vaginally. If this is the case, the doctor will need to make a small incision beneath the belly button called the mini-laparotomy.
Post Tubal Ligation/PTLS Syndrome
Photo by: Bruce Blaus/ CC BYThis is important to consider. Around 37 percent of women experience post-tubal ligation syndrome. Many different symptoms can be correlated with health problems, so making the connection between symptoms and those related to post-tubal ligation syndrome. Symptoms of post-tubal ligation syndrome include loss of libido, excessive headaches, IBS, breast tenderness, fatigue, weight gain, and abnormal periods.
Before becoming concerned with the possible side effects of tubal ligation surgery, it is important to recall that symptoms connected to the syndrome are also symptoms connected to the menstrual period. Making a permanent change to your reproductive system can impact your periods. Tubal sterilization surgeries have been said not proven to increase the pain and flow of blood during a period as well as ovulation cramping. This surgery will not impact the hormones. However, landmark research published in the Southern Medical Journal has compared women post-surgery menstrual cycle or stages, taking previous birth-control methods to account as well.
Women who were on the pill reported more cramping, bleeding as well as other symptoms post the surgery. Women on intrauterine devices reported less and women using barrier methods such as diaphragms reported no changes in the amount of cramping, blood release or associated symptoms. There’s need to counsel women on pills who want their tubes to be tied for taking oral contraceptives to see what periods will be like. If a woman experiences problems and takes pills to regulate her cycle as well as control other symptoms, surgery may not be an option. Much akin to laparoscopic operations, tubal ligation carries the likelihood of damage to the major blood vessel, bowel or bladder-type infections or hemorrhage.
CDC continues to study the long-term effects of post tubal ligation as women continue to raise awareness and demand answers. A woman contemplating the surgery should consider all options and be aware of possible risks. Post tubal ligation syndrome is a condition that is iatrogenesis oriented. It is often the result of a rapid fall in estrogen or progesterone hormone levels caused by blood supplies being damaged to ovaries during tubal ligation surgery.
Based on damage to veins and capillaries, blood volume to ovaries may fall or be completely eliminated known as an isolated ovarian syndrome associated with hysterectomy operations. Many symptoms of PTLS common with hysterectomy operations. Many symptoms of PTLS are associated with hormone shock, menopause, and estrogen or progesterone imbalance. Other symptoms like heavy painful periods can also be called by a hormonal imbalance and adenomyosis caused by uterus muscle and tissue being damaged, affected by tubal ligation surgery impairing the blood supply to areas of muscle or organs or a combination. Pain can also be the result of retro bleeding backing into fallopian tubes that are sealed.
Other theories of PTLS and hormonal imbalance results post a tubal ligation targeting receptor cells that are critical for the relay of hormonal messages are destroyed, damaged or removed at the time of the tubal ligation surgery. These receptor cells communicate, sending messages to the brain. The target or receptor cells are situated within the fallopian tube.
With this in mind, it is possible for women to have her ovaries still functioning to a degree if the blood supply was not damaged, have no major problems with the uterus, again if the blood supply was not damaged to that organ, and still be experiencing post tubal ligation syndrome in the form of hormonal imbalance led by changes in hormonal message related system due to receptor cells being removed.
The only way to find out if one has a hormonal or menopausal condition is to carry out effective hormone testing. Post tubal ligation syndrome is linked with severe hormone imbalance, ovarian isolation, atrophic ovaries, hormone shock, increased heart disease risk, bone loss and osteoporosis, dysfunctional uterine bleeding, post menstrual syndrome, endometriosis, severe pelvic adhesions, adenomyosis, misplacement of female organs, and decreased lactating ability.
Irregular periods include shorter or lighter periods, heavier periods, flooding, shorter/longer cycles and phantom periods. Loss of libidinal urges and changes in vaginal conditions, crashing fatigue, anxiety and feeling uneasy, disturbing memory losses, mental confusion, anxiety, feeling ill at ease are some of the other symptoms.